Part One
Model Overview
Reducing healthcare costs is a crucial step toward improving life expectancy and overall health outcomes in the United States.
Consider these striking statistics:
To explore potential solutions, this model estimates the cost savings of pre-hospital telehealth programs by applying findings from the 2016 study: “Cost Benefit Analysis of Telehealth in Pre-Hospital Care.”
Conducted in Houston, Texas, the study assessed the financial impact of the ETHAN telehealth system, which redirects eligible patients from expensive emergency services (ambulances and ERs) to more cost-effective alternatives (taxis and urgent care centers). [1]
Key Findings
Model projections for 2024 suggest that state-level cost savings from implementing similar programs could range from 2.48% to 16.22% of annual health and hospital expenditures, highlighting the transformative financial potential of pre-hospital telehealth adoption across the U.S. (Figure 1)
Figure 1
Methodology
A. Model Inputs
To simulate 2024 cost savings across 31 U.S. states, the model incorporates:
B. Patient Savings Calculation
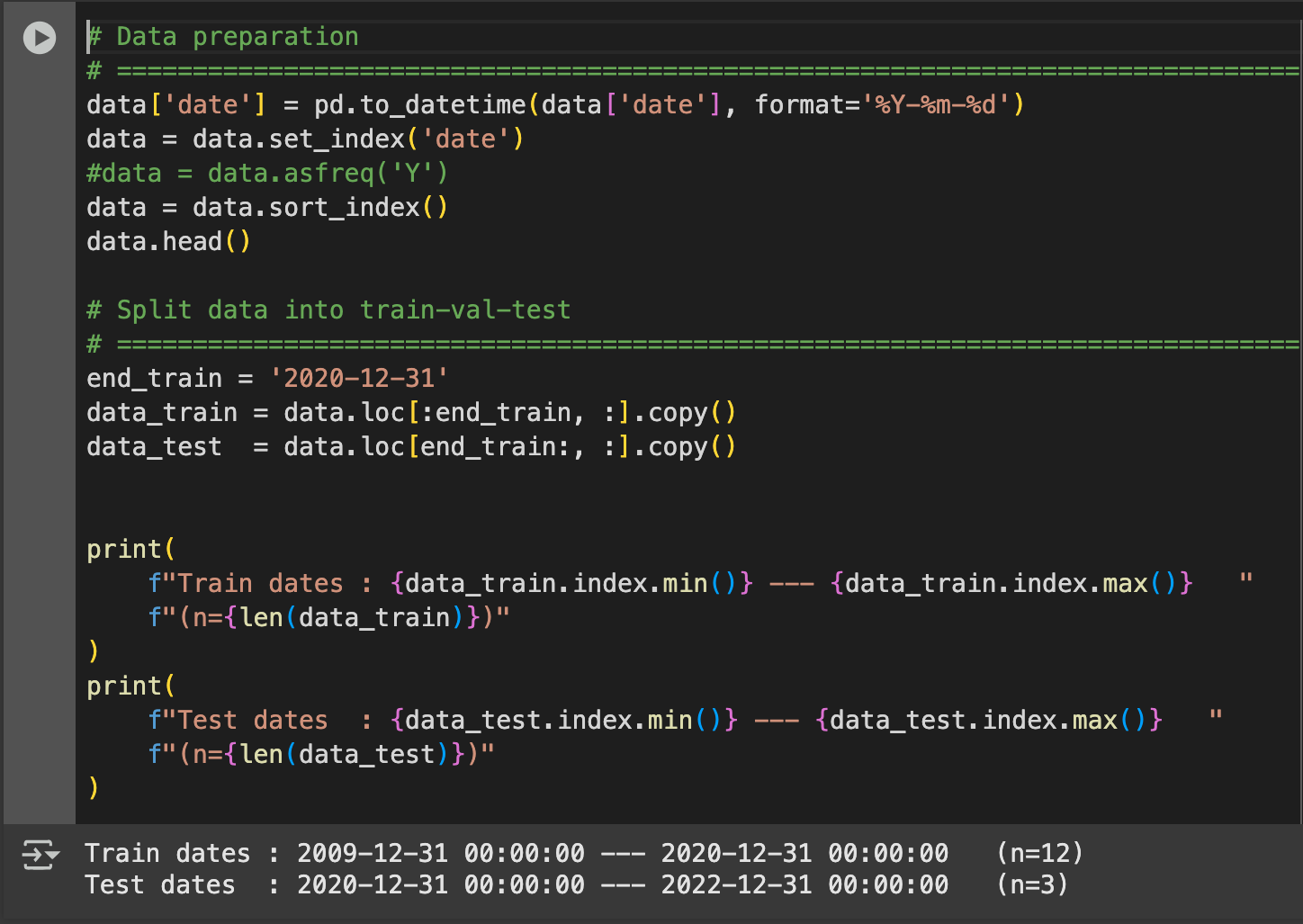
Total patient savings were determined by combining 2021 PCRED costs with state-specific ED visit data. Since Nevada’s ED visit data was unavailable, it was estimated using multivariate forecasting in Python.
Bi. Forecasting Emergency Department Visits
To estimate missing ED data, the model applies multi-series recursive forecasting, which accounts for underlying trends impacting state emergency department visits.
Figure 2
Short-Term Trend Analysis
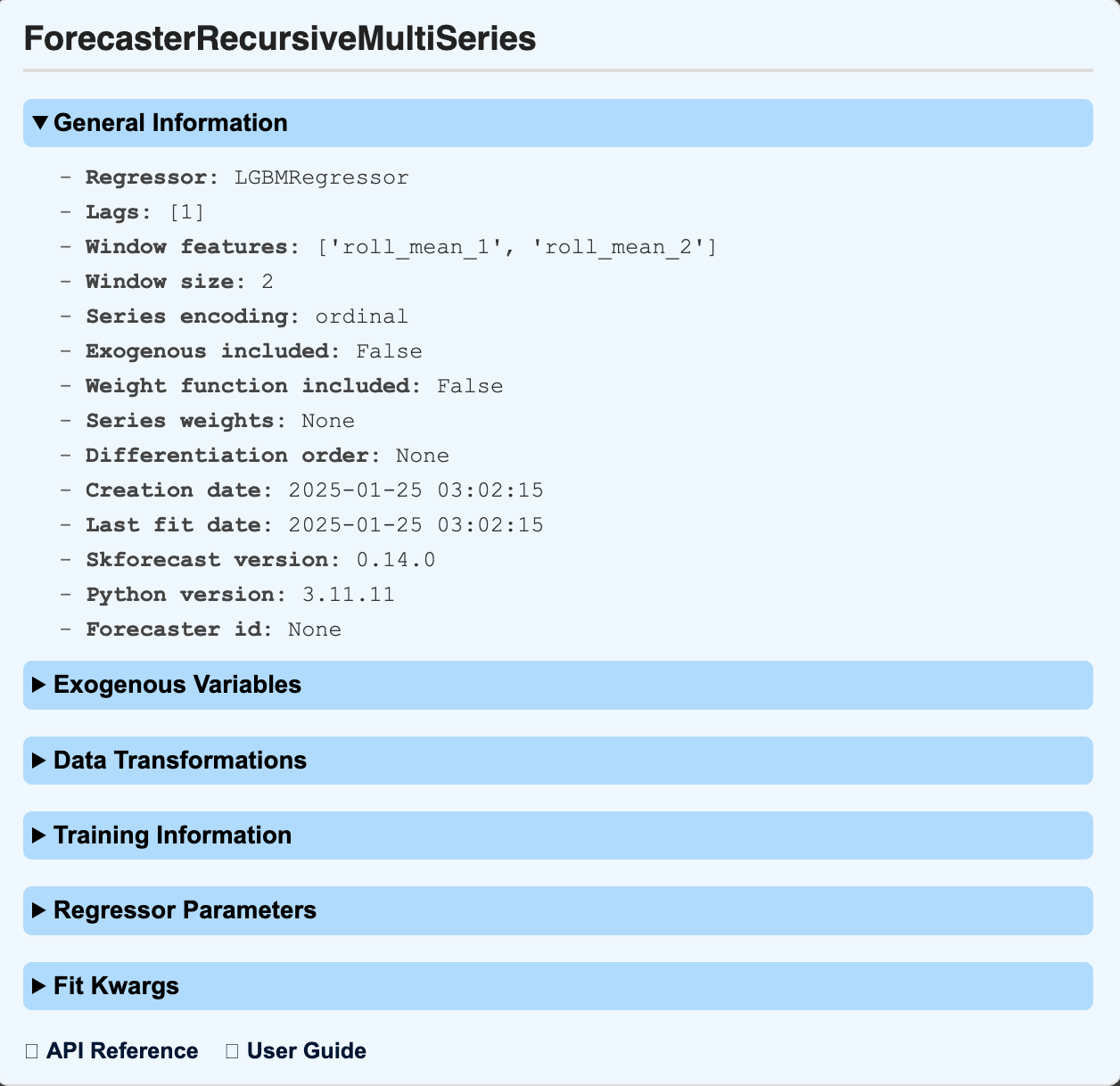
The model leverages the LightGBM recursive forecasting method with a lag of 1, ensuring each predicted year’s value informs the next. This technique captures short-term fluctuations, such as:
By using a shorter rolling window, the model preserves year-over-year variations instead of smoothing them out. (Figure 3)
Figure 3
Prediction for Nevada (2021 ED Visits):
C. Provider Savings Calculation
Provider savings were estimated using the ETHAN study’s $103 per-visit cost reduction.
- Adjusting for State Differences: The real price parity (RPP) index was used to scale Texas-based cost savings across 31 states.
- Forecasting Future Savings: The 2021 provider savings estimate was projected forward to 2024 using compounded annual healthcare inflation rates.
D. Combined Cost Savings
The final total cost savings per state was calculated by combining patient and provider savings (Figure 4).
Figure 4
Key Takeaways
By expanding telehealth solutions nationwide, the U.S. can reduce healthcare spending, enhance access to care, and improve long-term health outcomes.
Footnotes & Data Sources
(1)Total emergency department visit data was sourced from the State Emergency Department Database (SEDD), sponsored by the Agency for Healthcare Research and Quality (AHRQ).
Graphic: Deepai.org